Page 1, 2, 3
How to Diagnose Testosterone Deficiency
In my medical practice, I base my diagnosis of "testosterone deficiency" on the presence in a male patient of typical testosterone deficiency-related complaints and physical signs, and on laboratory tests of testosterone and its metabolites. In testosterone deficiency, the serum and urinary levels of the androgens are sufficiently low to be scientifically linked to higher risks of illness and death, but they might still be situated within the reference range. Also, to confirm the diagnosis, I prescribe a trial of testosterone therapy. If, during this treatment trial, the male patient loses his testosterone-deficiency complaints and physical signs, and he shows no overdose effects at physical examination and in laboratory tests, I consider the diagnosis confirmed and that the testosterone treatment is justified, safe, and efficient.
Typical Complaints of Male Hormone Deficiency
Table 1 below lists the most common symptoms that show testosterone deficiency in men.
- A persistent fatigue from awakening till bedtime, which worsens with physical activity
- Poor or reduced physical performance, including in sports
- Joint pain during physical activities
- A grumpy mood that may develop into depression and is also present from morning to night
- A tendency to quickly run short of breath during physical effort
- Easily inflamed tendons (e.g., in knees and heels – inflamed Achilles tendons)
- An anxiety state wherein details can be dramatized
- A tendency to be overweight with abdominal obesity (belly fat)
- Hot flashes, especially during meetings or at other stressful moments
- Excessive hesitations, difficulty making decisions
- Loose and atrophied muscles
- Lower sex drive
- A lack of determination, initiative
- A lax and obese body
- Erectile dysfunction characterized by a decrease in frequency of erections, especially morning erections84-86
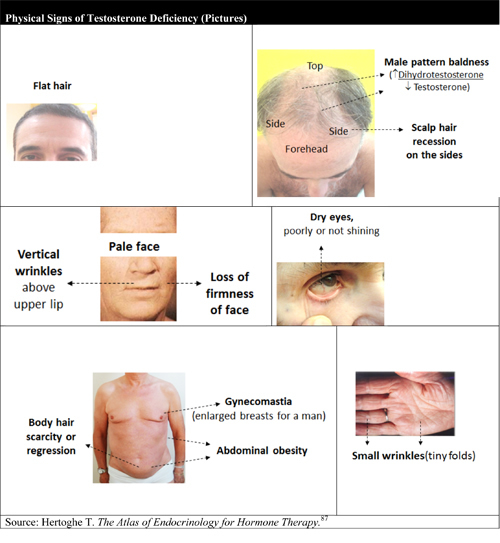
What are the typical physical signs of male hormone deficiency?
Table 2 gives examples of the physical signs of testosterone deficiency in men.
Laboratory Tests Needed and How to Interpret Them
A series of tests confirm the diagnosis of testosterone deficiency.
At the initial assessment, I often ask for the following laboratory tests:
- Total, not free, testosterone serum level. Test kits for free testosterone, which is not bound to a plasma-binding protein in the blood and easily penetrates by diffusion into target cells, are often of poor quality and unreliable. The better, more stable test is that for total testosterone, which measures all of the testosterone molecules found in the blood, those bound to transporting proteins and those in free form.
- Androstanediol glucuronide: This is the major metabolite of dihydrotestosterone. A metabolite is what remains of a hormone after it has exerted its action. High levels of androstanediol glucuronide signify that dihydrotestosterone activity is abundant in the body and that the male patient may be sexually very active (especially having good ejaculations) and have a clearly defined masculine physical appearance. It may also reflect a higher risk of male pattern baldness and body hair overgrowth.
- FSH (follicle stimulating hormone), the pituitary hormone, whose mission is to stimulate spermatogenesis. With age, its level increases to stimulate sperm production, which progressively declines with age. Unfortunately, as FSH also stimulates estradiol production, high FSH levels may produce excessive levels of estradiol. With aging, the increase in the FSH serum level is one of the first strong indicators of testicular failure. It usually precedes the age-related increase in LH (luteinizing hormone, the pituitary hormone that stimulates testosterone production).
- SHBG (sex hormone-binding globulin): I absolutely recommend checking the SHBG, the main transporter protein for male hormones. Finding a higher SHBG level (at or above the average level of the reference range) in the presence of a – for young men – average testosterone level signifies that there is a testosterone deficiency, as excessive amounts of this protein in the blood usually bind too strongly to testosterone molecules, preventing most of the testosterone from leaving the blood and penetrating the target cells.
- In addition, I recommend checking the blood levels of female hormones, especially estrogens, estradiol in particular, and sometimes estrone and progesterone. This is because estrogen excess reduces the efficacy of testosterone by blocking testosterone receptors and by stimulating metabolic reactions that oppose those of testosterone. A low progesterone level allows men to accumulate estradiol. High levels of progesterone are necessary in men to deactivate estrogens by stimulating the conversion of potent estradiol to estrone, which is 3 to 10 times less potent.
- Other tests: LH (luteinizing hormone), the pituitary hormone that stimulates testosterone and progesterone production; prolactin, the pituitary hormone that at high levels reduces testosterone production.
Treatment of Testosterone Deficiency
There are various types of testosterone formulations to be taken sublingually, orally, transdermal, or intramuscularly. The most common formulation that I prescribe to my patients is a transdermal liposomal gel of testosterone at a concentration of 10% (100 mg per gram of testosterone). Doses are between ½ and 3 g/day.
Why not use the pharmaceutical brands of testosterone gel available in prescriptions at any pharmacy?
The usual brands of testosterone gels at 1% take more time to apply (per 5 grams) and are just too poorly concentrated to reach satisfying levels in most patients. The persistence of pharmaceutical companies in keeping concentrations low is explainable: a desire to avoid at all costs getting their names cited with regard to testosterone abuse by athletes. |
Liposomal formulation makes testosterone penetrate the skin better.
Correct use of a transdermal testosterone gel
• How to proceed? Apply the testosterone gel to the skin in four successive thin layers by intensively rubbing the testosterone into the skin in between the application of each new layer. When a thin layer of testosterone is applied, the alcohol of the gel easily evaporates, and the evaporation cools the skin, which reacts by the vasodilatation of the arteries and the opening of the capillaries in the skin. This stimulation of the skin's blood vessels helps the skin to absorb the testosterone more effectively. Applying a thick layer of the testosterone gel to the skin does not permit the alcohol to evaporate and open up the blood vessels. Furthermore, the alcohol that remains on the skin – imprisoned in the thick layer – dries the skin and irritates it.
• Where to apply? Apply the testosterone gel to hairless skin with high absorption capacity, such as the forehead, the sides of the neck, and above the collarbones – areas where we flush with emotion because of their greater number of blood vessels, thereby facilitating absorption.
• Avoid hairy areas. Avoid applying the testosterone gel to areas with a lot of body hair, such as the beard or a hairy chest. Otherwise, the testosterone will turn into dihydrotestosterone, the male hormone that promotes body hair growth but makes men lose scalp hair. Hairy areas, such as the beard and mustache, for example, are rich in 5-alpha-reductase, the enzyme that converts testosterone into dihydrotestosterone. |
A second form of testosterone also provides satisfaction: intramuscular (IM) testosterone injections. IM injections are more appropriate for older men (above 60 years), whose skin does not absorb testosterone well. The use of injections assures that all testosterone enters the body. These injections can be applied daily, biweekly, weekly, every 10 days, every 2 weeks, or once every 6 to 8 weeks depending on the preparation.
The best effects are obtained, in my experience, with testosterone enanthate or testosterone cypionate, which both have similar duration in biological activity – 10 to 14 days before the effects die off and testosterone has dropped back to the initial level. However, the effects are even better when the products are injected in divided doses at a higher frequency, every week or twice a week, or in enthusiasts, every day or two days. The logic behind this is that higher-frequency injections provide more stable levels. Most patients learn to self-inject these high-frequency IM injections in the mid-thigh (external side: vastus lateralis muscle). When the 150 to 250 mg of long-acting testosterone are injected every 2 weeks, the first 5 days after injection, testosterone levels are usually excessive with levels well above the upper reference limit and, in some, with overdose symptoms and signs (erythematous face, oily hair and skin, acne, excessive sensitivity to sexual stimuli, etc.), whereas 10 to 14 days after injection, the testosterone level tends to drop too low, at levels well below optimal levels. Approximately a quarter to a third of patients may feel testosterone deficient on those last days before the next injection.
 Men who prefer to get their injections with greater intervals can get testosterone undecanoate injections of 1000 mg every 6 to 8 weeks. The frequency of every 3 months proposed by the pharmaceutical firm that produces them is for most testosterone-deficient men too long, as the testosterone level has then dropped in them back to the initial low pretreatment levels. Male patients feel testosterone deficient during the third month in this situation. Testosterone pellets provide satisfying beneficial effects and are also an alternative for those patients who do not want to bother too much with treatment. A pellet can be implanted every 3 to 4 months and let the patient enjoy stable levels, but this form does not permit the elevating of the dose in transient periods of increased need (intensive sports, for example). In those cases, the daily transdermal testosterone gel is more indicated. Men who prefer to get their injections with greater intervals can get testosterone undecanoate injections of 1000 mg every 6 to 8 weeks. The frequency of every 3 months proposed by the pharmaceutical firm that produces them is for most testosterone-deficient men too long, as the testosterone level has then dropped in them back to the initial low pretreatment levels. Male patients feel testosterone deficient during the third month in this situation. Testosterone pellets provide satisfying beneficial effects and are also an alternative for those patients who do not want to bother too much with treatment. A pellet can be implanted every 3 to 4 months and let the patient enjoy stable levels, but this form does not permit the elevating of the dose in transient periods of increased need (intensive sports, for example). In those cases, the daily transdermal testosterone gel is more indicated.
Sublingual testosterone forms are less efficient and need to be taken twice a day. Oral testosterone formulations are often poorly absorbed. Almost all of the testosterone is broken down in the liver after absorption before it can penetrate the blood. To avoid this breakdown, one pharmaceutical company markets oral capsules of testosterone undecanoate, which is for a small part absorbed through lymphatic vessels, avoiding the liver. This form is more active and may provide satisfactory results to young men with milder forms of testosterone deficiency.
Page 1, 2, 3 |
![]()
![]()
![]()






