Page 1, 2, 3, 4
The fourth case (Tower, 1960) involved a 13-year-old boy with petit mal seizures. During 18 months on L-asparagine and paramethadione, he was having approximately 230 seizures each month. GABA was taken exclusively; and during the 19-month observation period, the frequency of seizures reduced to around 70 each month (Figure 3). Based on the aforementioned results, Tower (1960) noted the following:
These four patients demonstrate that daily oral administration of GABA can be an effective anticonvulsant, and it can appropriately prove effective against various different types of seizures. The seemingly readier response of the minor or petit mal types cannot properly be evaluated on such a limited number of patients (p. 571).
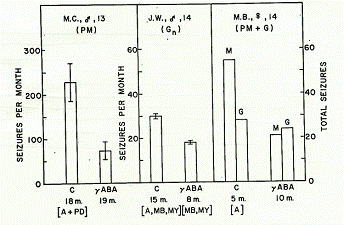
Figure 3. Seizure frequencies for three patients during control (C) periods
and periods on oral GABA 2 mM/kg 4 times daily. Observation periods
in months (m) indicated below each bar. For two patients on the left seizures
are plotted as mean frequency per month for each period with the standard
deviations indicated by the central line atop each bar. For patient M. B. on the
right seizure are plotted as total number for the entire respective observation
periods. (Abbreviations: Seizure types: PM= petit mal; Gn=nocturnal generalized
or major; G=generalized or major; M=minor or petit mal; medications during control
periods: A=L-asparagine; PD=paramethadione; MB=mephobarbital/Mebaral; MY=Mysoline).
(Tower, 1960, p. 571). Reprinted with permission from: Tower, D. B. (1960). The
administration of gamma-aminobutyric acid to man: Systemic effects and anticonvulsant
action. In Inhibition in the nervous system and gamma-aminobutyric acid (pp. 562-578).
New York, NY: Pergamon Press, Inc.
Tower (1960) also noted that there were other cases, however, where the use of GABA did not result in any reduction in seizure frequency. He described a 35-year-old man with petit mal-type seizures who took GABA for almost 2 years without any change in seizure frequency compared to an earlier control period when GABA was not taken. There was a 16-year-old girl with petit mal-type seizures primarily occurring with menstruation, who did not experience any clinically significant benefit from GABA over a six-month period of observation. Regarding other patients who also underwent brief trials of GABA but did not respond, Tower commented:
Regardless of factors perhaps peculiar to GABA, these differences in clinical response are not too surprising, since there is no known anticonvulsant which has proved effective in more than about two-thirds of a given epileptic population (p. 572).
GABA and Phosphatidylserine
A study evaluated supplemental GABA and phosphatidylserine (PS) among teenage and adult patients (age range: 15-65; n=42) with various forms of epilepsy (Loeb et al, 1987). These orthomolecules were used because anti-seizure activity was previously demonstrated when they were administered parenterally in a liposomal suspension in different seizure models and when they were administered separately to rats. The oral forms of GABA and PS were studied because, as the authors noted, they were readily available and shown to be safe for human consumption. Only 34 patients completed the study. All patients in this study were on one to three anti-seizure medications. There were three separate trials in the study, denoted as Trials A, B, and C.
Trial A (n=12) determined if combining anti-seizure medication with the supplements resulted in any alteration in the plasma levels of anti-seizure medication, with titrating doses of GABA (from 1,500-2,500 mg/day) and PS (from 300-500 mg/day). The results of Trial A did not demonstrate any statistically significant alteration in the plasma levels of anti-seizure medication.
Trial B (n=10) utilized a double-blind procedure in assessing the efficacy of the supplements (i.e., 2,500 mg/day GABA and 500 mg/day PS) over a treatment duration of three months.
Trial C utilized a single-blind procedure over a treatment duration of eight months in assessing the efficacy of the supplements (i.e., 2,500 mg or 3,000 mg of GABA daily, either dose in combination with 500 mg/day PS). All patients in Trials B and C were considered to have responded when there was a 50% or more drop in the mean monthly seizure frequency compared to the respective reference periods and/or placebo periods.
The results (Loeb et al, 1987) showed significant clinical improvements, with 10 patients from the 34 (29.4%) having a demonstrable drop in seizure frequency (expressed as mean number of seizures per month ± SD) of 50% or more. When the results were analyzed more closely, only the patients with absence seizures (AS) showed statistically significant differences from the reference period and placebo, and clinically significant differences in monthly seizure frequency. A total of 12 patients with AS were analyzed separately to determine their response to the supplements. With respect to Trial A (n=5 with AS), there was a clear dose-response relationship demonstrating a drop in seizure frequency with increasing doses of GABA and PS. When combining Trials B and C (n=7 with AS), there were statistically significant, as well as obvious clinical differences, between treatment versus the reference period, and treatment versus placebo. There were statistically significant decreases in the mean number of seizures per month when comparing the reference period (22±16) and placebo (16±12) to that of treatment (5±9). When Trials A, B, and C were combined (n=12 with AS), the results demonstrated a statistically significant drop in the mean numbers of seizures per month during the reference period (29±18) and treatment period (12±13).
Adverse effects were considered minimal and of no clinical concern (Loeb et al, 1987). Only one patient experienced significant gastric distress and dropped out, two patients experienced nausea, four patients had drowsiness, one with constipation, and one with a brief spell of amenorrhea. No changes in lab values were evident in 37 patients, but five did have minimal increases in alanine aminotransferase and decreases in fibrinogen and prothrombin time. The authors concluded that the combined use of GABA and PS "brought about a significant decrease in absence seizures, while complex partial seizures showed no significant changes" (pp. 211-212). Even though the results were considered to be very preliminary, the authors mentioned that there is a rather urgent need to further study the therapeutic effects of GABA and PS among subjects having AS.
Another report on the combination of GABA and PS was published by Cocito, Bianchetti, Bossi, Gilberti, & Loeb (1994). They investigated the anti-seizure properties of this combination in nine patients with seizures associated "with an EEG pattern of photoconvulsive response at intermittent photic stimulation" (p. 49). They administered GABA (3,000 mg) and PS (600 or 1,200 mg) once orally and then assessed for any changes that would suggest anti-seizure activity among the study subjects exposed to intermittent photic stimulation. They concluded that a single dose of this combination was ineffective but that chronic administration may be required to demonstrate benefits. What was surprising about this study was that all the prior research related to seizures and GABA and/or PS had clearly demonstrated benefits only from chronic and not from acute administration. This study was not methodologically well constructed from the outset; and given the outcomes from previous research, there was little probability that the single-dose administration of the GABA-PS combination would demonstrate any significant clinical effects.
With respect to adverse effects from PS (those from GABA have already been discussed), PS has a tremendous safety record and produces rare stomach upset when large daily doses are used (e.g., 600 mg), or possibly sleeplessness if taken immediately before bed (Kidd, 1996). Otherwise, numerous clinical trials on more than 800 patients have shown PS to be very safe and well tolerated (Kidd, 1996).
Putative Mechanisms of Action
Based on the clinical data presented thus far, it is evident that GABA and the GABA-PS combination represents a novel complementary approach to the treatment of AS. With respect to how GABA exerts its therapeutic effects, Tower (1960) reported that there did not seem to be any strong connection between the reported therapeutic responses to GABA and its levels in the blood and cerebrospinal fluid. When commenting further, he noted that any "direct response between body fluid levels and therapeutic response should not necessarily be expected for a compound like GABA, which if it does penetrate from blood into the central nervous system, might pass directly to the tissues rather than into cerebrospinal fluid" (p. 574). Lastly, he mentioned that given the possibility that epilepsy represents a condition associated with increased blood-brain-barrier permeability, there is also the possibility of increased cerebral penetration of "systemically administered GABA" (p. 575).
Modern research has attempted to better understand how GABA exerts its effects on the central nervous system. In a study (Abdou et al, 2006) that assessed GABA's effects upon relaxation and immunity, a mere 100 mg orally resulted in EEG changes associated with increased alpha waves and decreased beta waves among healthy volunteers. These effects were more significant than EEG alterations associated with water and L-theanine administration. These results suggested that GABA possesses anxiolytic and relaxation effects mediated by alterations in brain wave activity. In another study (Yoto et al, 2011), responses to mental stress was evaluated among healthy adults given 100 mg of GABA orally or placebo. GABA abrogated the drop in alpha and beta brain waves following mental stress. The subjects on placebo had more marked declines in their alpha and beta brain waves compared to the brain-wave declines among the subjects taking GABA. Changes in the "vigor-activity" scores of the Profile for Mood States questionnaire among the subjects on GABA were less pronounced than those associated with placebo, which reflected a potential benefit upon mood or a subjective anti-stress effect from the orthomolecule.
A study among healthy human volunteers (Fujibayashi et al, 2008) demonstrated that following an overnight fast, the oral use of GABA (precise dose unspecified) resulted in increased autonomic nervous system and parasympathetic nervous system activity. While I was not able to read the actual study since it was published in Japanese, the abstract in English reported that these positive changes were attributed to alterations in heart rate variability.
Another study assessed GABA and Apocynum venetum leaf extract (AVLE) to assist with sleep among 16 subjects suspected as having some type of sleep disorder (Yamatsu et al, 2015). The subjects were either given GABA alone (100 mg), AVLE alone (50 mg), or GABA (100 mg) combined with AVLE (50 mg) 30 minutes prior to bed. EEG and other measurements were taken. GABA administration resulted in shortened sleep latency by 5.3 minutes (i.e., with a trend toward statistical significance), and also reduced non-REM sleep latency but these latter findings did not reach statistical significance. These results, according to the authors, "suggested that GABA had an effect to help people to fall asleep quickly and easily" (p. 184). The mechanism underlying these effects on sleep were attributed to GABA's role as an inhibitory neurotransmitter in the central nervous system.
In a review article, "Neurotransmitters as food supplements: The effects of GABA on brain and behavior,"the mechanism of GABA was thoroughly discussed and debated (Boonstra et al, 2015). The article mentioned the controversy about whether or not GABA crosses the blood-brain-barrier and raised some important possibilities to account for GABA's observed therapeutic effects. First, there is a GABA-transporter in the blood-brain-barrier, which means that GABA enters or exits the brain through facilitated transport. Given the fact that in mice the influx rate was found to be much slower than the efflux rate, there is the possibility that in humans GABA gains entrance into the brain but is quickly moved out because of the very high efflux rate. This would make it extremely difficult to measure the amount of GABA in the central nervous system following oral administration because of the very high efflux rate. Second, there is the possibility that GABA works better among younger individuals because some evidence suggests that blood-brain-barrier permeability reduces with age. So perhaps younger patients such as children and teenagers would respond better to GABA given their presumably more permeable blood-brain-barriers. Lastly, GABA might exert its effects indirectly via the enteric nervous system even though the relationship between "the oral administration of GABA, the vagal nerve and GABA levels in the brain has not been established yet" (p. 4).
With respect to PS, animal research has evaluated the effects of PS and GABA co-administration via parenteral routes. One report, for example, demonstrated that the acetylated derivative of PS (i.e., lysophosphatidylserine; LS) possessed anticonvulsant effects against isoniazid-induced seizures in mice (Toffano et al, 1984). The anticonvulsant effect of LS was present in the absence of GABA but was also shown to enhance the anticonvulsant effects of GABA when they were co-administered. In a rat study, both GABA and PS were found to possess no seizure activity when administered alone; but when co-administered, they significantly reduced the number of spikes among rats with penicillin-induced seizures (Loeb et al, 1985). Another report on rats (Benassi et al, 1992) demonstrated that when PS was co-administered with GABA, there was a resultant increase in the synaptic availability of the neurotransmitter, thus increasing the supply to GABA-ergic nerve endings. These findings suggest that PS might possess anti-seizure effects on its own, but most likely augments the anti-seizure effects of GABA when they are co-administered. Ultimately, however, PS exerts broad-spectrum effects that influence nerve cell membrane functionality by optimizing a variety of homeostatic processes - such as the entry of micronutrients into neurons, and energy production by functioning as a metabolic backup to other phospholipids (Kidd, 1996).
Discussion
It is apparent that some patients with AS will benefit when GABA or GABA-PS are combined with standard anti-seizure medication. The earlier work on GABA used tremendous daily doses (0.8 g/kg) to achieve positive therapeutic effects. Such a high daily dose would likely be difficult for most patients to sustain over extended periods of time, and the monthly costs could be prohibitive. It appears that PS augments the anti-seizure effects of GABA, which allows for a much smaller daily dose of GABA without compromising clinical efficacy. This would be much easier to comply with over extended periods of time and be more affordable. When reviewing all the clinical data, GABA and GABA-PS represent novel complementary approaches to the management of AS (formerly classified as petit malseizures), and possibly other types of generalized seizures. Table 2 contains a summary of all the published results, which clearly point to a very tolerable, safe, and potentially effective treatment.
Table 2. Clinical Response to GABA and GABA-PS among Patients with Absence Seizures |
Intervention |
Daily dose |
Clinical outcome |
GABA |
0.8 g/kg |
Significant reduction in monthly seizure frequency among 4/11 patients (36%; Tower, 1960). |
GABA-PS |
3,000 mg GABA; 500mg PS |
Reduction in monthly seizure frequency of 50% or more in 10/34 patients (29.4%); 12 patients with AS showed the most marked clinical response with a statistically significant drop in the mean number of seizures per month (29±18 during the reference period to 12±13 during the treatment period; Loeb et al, 1987). |
Page 1, 2, 3, 4 |
![]()
![]()
![]()
![]()





