|
Page 1, 2
Changes in Muscle Strength: A Critical Element in Tension-Type and Cervicogenic Headaches
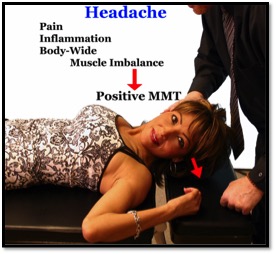
A high percentage of headaches can be corrected with treatment determined by manual muscle testing (MMT) examination. Thorough knowledge of the mechanism(s) causing the cervicogenic or tension-type headache is important because there often are limited objective findings, especially during the pain-free period.1 It should be recognized however that muscle imbalance has clearly been measured as a fundamental characteristic of musculoskeletal pain syndromes involving the head and neck.2-6 The manipulative treatment of muscle imbalance physiology was first elaborated by Dr. George J. Goodheart, Jr.6 Muscles predictably respond with weakness to pain, inflammation, and/or injury. (Figure 1)
Figure 1
MMT makes it possible to diagnose this fundamental component of tension-type or cervicogenic headaches |
 |
With a lifetime prevalence of 93% in men and 99% in women, headaches are undeniably an extremely common problem.7 Women consistently reported neck pain 83% more than men in a review of 25 studies by Dennison & Leal.8 With a prevalence of over 47% reported in some populations, episodic tension-type headache is the most common of all headache types; chronic tension-type headache is found in 1% to 3% of the general population.9 However, its prevalence may be as high at 15 to 20% in those with chronic headaches.10
 Townsend Letter provides a platform for those examining and reporting on functional and integrative medicine. Please support these independent voices. Townsend Letter provides a platform for those examining and reporting on functional and integrative medicine. Please support these independent voices. |
Given the co-variance of muscle inhibition found in patients with headaches and the cost of headaches to both individuals and society at large, it cannot be stressed enough that MMT should become part of every clinician's assessment of patients with headache.
 In patients with cervicogenic or tension-type headaches, there are specific and measurable motor control losses that can be assessed, identified and become the focus of therapeutic interventions. Applied Kinesiology is a system that suggests that muscle dysfunctions arising from, or part of the etiology of cervicogenic headaches, should be recognized and corrected as part of the over-all treatment strategy. In patients with cervicogenic or tension-type headaches, there are specific and measurable motor control losses that can be assessed, identified and become the focus of therapeutic interventions. Applied Kinesiology is a system that suggests that muscle dysfunctions arising from, or part of the etiology of cervicogenic headaches, should be recognized and corrected as part of the over-all treatment strategy.
Substantial research has shown how general functional ability can be measured with simple, reliable, inexpensive, time-efficient tests…tests that have obvious "face-validity."11 MMT qualifies on each of these counts. If a test has good 'responsiveness', then the test results should improve as a person's health status improves. MMT has shown excellent responsiveness because it accurately shows change when it has occurred in the patient.12 Like a light dimmer switch, muscle strength is thought to be turned down by the central nervous system in order to unload and protect the sensitive or damaged tissues.13 Manipulative treatment to these damaged or sensitive tissues corrects the motor control problems found in these patients.12, 14-15
Alterations in Cervical Motor Control
Briefly, the following data emerges from the current literature concerning the muscular inhibitions co-present in patients with tension-type or cervicogenic headaches and neck pain:
- Reduced force of contraction: In agreement with observations in people with neck pain, cervicogenic headache sufferers demonstrate deficits in the strength of the muscles producing cervical flexion and extension or cervical flexor muscles, the longus colli and longus capitis.16-23
- Reduced range of motion: Reduced range of motion, usually due to muscle inhibition, is well documented in these patients; and current classification criteria for cervicogenic headache include restricted range of motion of the cervical spine.16-17, 24 Individuals with high pain-related fear also have smaller excursions of cervical spine.
- Decreased proprioceptive acuity with neck and headache pain.25‑26
- Decreased endurance of muscles: Increased fatigability of craniomandibular and axioscapular muscles in patients with cervicogenic headache and neck pain.22, 27-28
- Alterations in timing of muscular contraction and impaired coordination control of muscles as well as cervical joint coordination are each altered in headache patients.29-30
- Impaired balance and decreased postural stability: Changes in postural control in migraine and neck pain patients.31-32 Impaired postural control of the axioscapular muscles is associated with delayed muscle response times in neck pain patients.33 Cervical muscle pain changes feed-forward postural responses of the muscles throughout the body.34-35
- Impaired reaction time: Compared to healthy controls, persons with cervicogenic headache exhibit a reduced ability to adapt spinal muscle coordination and activity and show a slower reaction time.36
 Similar lists are available of contemporary research showing the muscle inhibitions accompanying most ofthe other physical disorders experienced by patients who visit physicians around the world.12, 28, 37-41 Similar lists are available of contemporary research showing the muscle inhibitions accompanying most ofthe other physical disorders experienced by patients who visit physicians around the world.12, 28, 37-41
The author recently showed that in a symptomatic group of patients with mechanical neck pain (148 patients) demonstrated significantly increased MMT findings in the form of reduced strength levels compared to a control group (100 patients).16 Weaknesses were broadly and to a large extent equally distributed (32.4%-43.2%) across the four muscle groups tested. (Table 1)
This evidence suggests that MMT is potentially a sensitive and specific test for evaluating cervical spine muscular impairments in patients with mechanical neck pain. Using a 95% confidence interval, we estimated that between 88.8% and 97.2% of all patients with mechanical neck pain have positive MMT findings in one or more of the four muscle pairs tested.
Table 1. Number and Percentages of Patients with Positive MMT findings, by Muscle Group
| |
Control Group |
Mechanical Neck Pain Group |
| |
(100 patients) |
(148 Patients) |
| Sternocleidomastoid |
18 (18%) |
61 (41.2%) |
| Anterior scalene |
13 (13%) |
49 (33.1%) |
| Upper trapezius |
4 (4%) |
64 (43.2%) |
| Cervical extensors |
2 (2%) |
48 (32.4%) |
In a second paper the author again investigated the prevalence of positive MMT findings for 52 patients with headache according to the International Classification of Headache Disorders.42 Muscle dysfunctions (inhibition) were found to be associated with headache (HA) in these patients as follows:
Table 2. Number and Percentages of Patients with Positive MMT findings, by Muscle Group with Headache (52 Patients)
Sternocleidomastoid.................................. 42 (81%)
Anterior scalene........................................ 24 (46%)
Upper trapezius......................................... 24 (46%)
Deep neck flexors..................................... 33 (63%)
In this group of 52 patients with HA, 49 patients had cranial dysfunctions that when treated with applied kinesiology improved all or a portion of the muscle inhibitions, while the initial Numeric Pain Scale of Neck and Associated Head Pain simultaneously fell from an average of 6.75 to an average of 0.49. Odds ratios were calculated to be >1, meaning there was a positive correlation between positive MMT of these muscles (as well as upper cervical and cranial dysfunctions), and headaches in this cohort. The evidence of this study suggests that MMT is a potentially useful diagnostic tool for evaluating peri-cranial muscular impairments in patients with both cranial dysfunctions and headache.
Tension-type or cervicogenic headache being associated with muscle inhibition and motor impairments is not a new concept. However, in recent years there has been an increase in the investigation of cervical motor impairment associated with headache. It is now known that cervicogenic headache sufferers present with an array of neuromuscular changes that are not unexpectedly different from those observed in people with neck pain.6, 16-17
In 1920 Cyriax first described the relationship between muscle weakness (detected with MMT) and headaches.21 In 2008 an important literature review on neck muscle strength by Dvir confirmed that "overall studies indicate that, compared to normal subjects, patients suffering from neck-related disorders present with significant reductions in cervical muscle strength."16-28
In 1991 Lund et al.28 described the pain adaptation model, reviewing the muscular changes in five chronic musculoskeletal pain conditions (muscle tension headache, TMJ dysfunction, fibromyalgia, chronic lower back pain, and post-exercise muscle soreness). Lund determined that these types of musculoskeletal pain disorders are not due to the older model of pain-spasm-pain cycle; instead, these conditions are mediated by the CNS as inhibition of the agonists and hypertonicity of the antagonists. Deficits in strength, endurance, and increased fatigability have been consistently demonstrated in the muscles that attach to the cranium in patients with whiplash-associated disorders, neck pain; and headache, using many different muscular assessment techniques.
It has been hypothesized that the powerful muscles attaching directly to the head and the cranial bones (which move rhythmically and in complex patterns) are capable of being specifically tested and treated.2-3, 12, 43
Manual Assessments in Tension-Type and Cervicogenic Headaches
Visual images of the manual muscle tests for headache and neck dysfunctions are presented below.
Falla has reported that both the sternocleidomastoid and anterior scalene muscles' strength were significantly reduced in patients with neck pain at 25% of maximum voluntary contraction (p<0.05).44
Recent studies by Nederhand et al have confirmed that cervical muscle dysfunction appears to be a general sign in diverse chronic neck pain syndromes, especially related to whiplash injuries.45-46 These studies suggest that the performance of the upper trapezius muscle is an invaluable diagnostic measurement in the evaluation of patients with chronic neck pain and chronic whiplash-associated disorders.
Cervicogenic headaches involve not only altered biomechanics, psychosocial anxieties, as well as significant costs to society, but also measurable motor control errors and local as well as remote muscular dysfunction that are part of the nervous system's response to pain and dysfunction.
If we are not capable of diagnosing this fundamental problem in patients with cervicogenic headaches, we are missing a fundamental component of their dysfunction making the treatment of complex neuromusculoskeletal disorders that much more difficult.
Page 1, 2
|
![]()
![]()
![]()
![]()








